Communication Frameworks and Professional Boundaries
How to discuss PEDs professionally without crossing into medical advice, manage documentation, set up physician referrals, and navigate the liability landscape of coaching in this domain.
- Distinguish between harm-reduction education and medical advice in the context of PED coaching
- Apply documentation practices that protect both coach and client
- Describe when and how to set up a physician referral without undermining the coaching relationship
- Manage client pressure for more aggressive approaches with clear, boundaried communication
- Understand the basic liability landscape and what coaches can and cannot do professionally
The Communication Problem Is a Boundary Problem
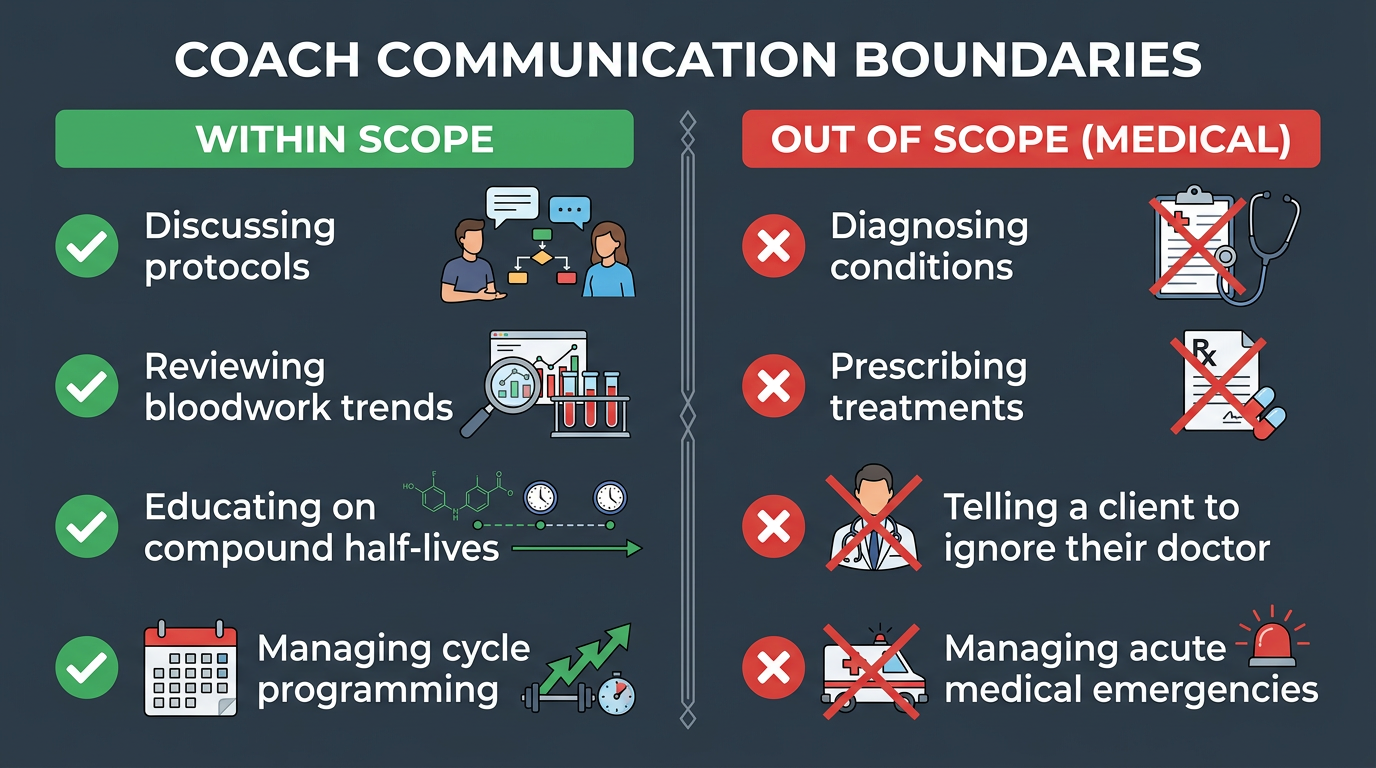
The most common professional failure mode for coaches in this space is drift, not malice. It begins with a legitimate educational conversation about Testosterone pharmacokinetics, ester half-lifes, and aromatization. It gradually expands to include opinions on dosing, then specific dose recommendations, then cycle design, then advice on managing side effects with AI adjustments. At no single step does the coach consciously decide to cross into medical practice. But somewhere in that progression they did, and if something goes wrong, the legal and ethical exposure is substantial.
Understanding where the line sits, and having a communication framework that keeps you on the right side of it consistently, is not a constraint on good coaching. It is a protection for both parties.
What a Coach Can and Cannot Do
The distinction between education and medical advice is well-established in healthcare ethics and law, though it is rarely applied to fitness coaching. The principle is this: describing how a compound works, what its documented effects and risks are, and how the existing literature characterises its use is education. Telling a specific individual what they should take, in what dose, for how long, or how to manage a specific symptom they are experiencing is medical advice.
A coach can explain that Trenbolone is a 19-nor androgenic compound with no approved human medical use, that it does not aromatize but can raise prolactin in susceptible individuals, that the cardiovascular risk profile is meaningfully higher than Testosterone, and that the harm-reduction literature recommends careful cardiovascular monitoring. That is education, well within the coaching role.
A coach cannot tell a client that they should run Trenbolone at 400 mg/week, that they need Cabergoline at 0.5 mg twice weekly to manage prolactin, or that their current side effect (whatever it is) is being caused by a specific compound and should be addressed with a specific intervention. Those are clinical judgments that require the ability to examine a patient, review their full history, order and interpret diagnostics, and take legal and professional responsibility for treatment decisions.
CompoundLab operates on the same principle. The platform provides compound profiles, interaction information, and educational content you can use to run informed conversations with clients. It is a reference tool, not a prescription generator. Use it accordingly: share a compound profile to help a client understand what they are considering, not to validate a cycle design you have created for them.
Documenting Conversations and Decisions
Documentation in coaching is most often associated with training programme design and progress tracking. In the context of PED-assisted coaching, documentation takes on additional significance: it creates a contemporaneous record of what was discussed, what information was shared, what the client understood, and what decisions they made autonomously.
At a minimum, your documentation practice should capture the following:
Intake record. The information the client provided during screening: bloodwork dates and key values, health history, age, training history, compounds they are currently using or considering, and any specific concerns or goals. This record shows you did your due diligence at the outset.
Education provided. Brief notes on what compound profiles, risk information, or educational resources you shared with a client at each session or interaction. “Reviewed Testosterone compound profile with client; discussed aromatization and the need for baseline bloodwork” is a more defensible record than no record at all.
Client decisions. Note that specific decisions about compound use were made by the client autonomously. You can frame this explicitly: “Client informed me they intend to begin a Testosterone Enanthate cycle at [their stated dose]. I reviewed the relevant harm-reduction information with them and referred them to a physician for bloodwork interpretation.” This framing documents your role as educator and referrer rather than prescriber.
Referrals. Any time you refer a client to a physician, note it in writing. Include the reason for the referral and whether the client followed through.
Digital tools, even a simple shared note or coaching journal, serve this purpose. The key is consistency. Documentation done after the fact or selectively loses most of its protective value.
Discussing PEDs Without Crossing the Line
The practical challenge is that clients want specificity. They want you to tell them what to use, not just explain how things work. Managing this dynamic while staying in role requires a consistent communication framework.
The most effective framework is the information-and-decision-separation model: your role is to make sure the client has accurate, accurate information; their role is to make the decision about what to do with it. This is how informed consent works in medicine. A physician who prescribes testosterone explains the mechanism, the expected benefits, the risks, the monitoring requirements, and the alternatives. The patient decides whether to proceed. You are providing a similar service at the educational level, without the prescribing authority.
In practice, this sounds like: “Here is what the research says about estradiol management on a Testosterone cycle. CompoundLab’s compound profile for Testosterone covers aromatization in detail. The decision about whether and how to use an AI is yours to make with your prescribing physician if you have one, or based on your own informed judgment if you don’t.” You have provided the education. You have not told the client to use Arimidex at a specific dose.
When a client asks a direct clinical question, “My estradiol came back at 82 pg/mL, how much [Arimidex] should I take?”, the appropriate response acknowledges the question and redirects without abandoning them: “That’s a value worth paying attention to. I can tell you that the CompoundLab profile and standard harm-reduction frameworks generally describe estradiol above 60–70 pg/mL as elevated and worth addressing. For specific dosing guidance on an aromatase inhibitor, that really needs to come from a physician who can look at your full panel and history, that’s outside what I can responsibly advise. Do you want me to help you find someone to consult with?”
This response is helpful, boundaried, and demonstrates genuine care. It does not leave the client stranded. It also does not expose you to liability for an AI dosing recommendation that might be inappropriate for this specific person.
When to Refer to a Physician
The physician referral is a routine part of professional practice. Any client using compounds should, ideally, have a physician who knows they are doing so and is willing to engage in informed bloodwork interpretation. many clients will not have this relationship, which is why your ability to identify when a referral is necessary and set it up effectively matters.
Automatic referral triggers include:
Any abnormal bloodwork the client reports. Your role is not to interpret bloodwork, it is to recognise that something looks abnormal and direct the client to someone who can interpret it properly. Liver enzymes above the upper limit of normal, hematocrit above 52%, estradiol significantly outside the reference range, LH and FSH remaining suppressed well post-cycle, all of these warrant physician evaluation before continuing.
Symptoms that may indicate a serious complication. Chest pain, significant dyspnoea (shortness of breath), unilateral leg swelling, signs of jaundice, severe headaches, visual disturbances, or anything that sounds like it might be cardiovascular or neurological in origin, these are emergency referrals, not routine ones. Tell the client to see a doctor immediately, not at their next scheduled blood draw.
Psychiatric symptoms. Significant aggression, depressive episodes, anxiety that feels new or out of proportion, or suicidal ideation (rare but documented) all require referral to a mental health professional immediately. Androgens have documented psychiatric effects, and a client going through a psychological crisis is someone who needs clinical support, not coaching frameworks.
Post-cycle recovery concerns. If a client’s HPTA is showing signs of prolonged suppression, total testosterone significantly below baseline at 10–12 weeks post-cycle, with ongoing low LH and FSH, they need physician guidance on whether a PCT extension, additional monitoring, or more active intervention is warranted. This is beyond the scope of coaching.
Making the referral well means more than saying “see a doctor.” Help the client identify what kind of physician is appropriate (sports medicine physician, endocrinologist, or an internist who is open to harm-reduction-informed conversation), what information to bring (their bloodwork, the compounds they have been using, the timeline), and what questions to ask. A client who arrives at a physician’s office informed and prepared gets substantially better care than one who presents vaguely.
Managing Client Pressure for More Aggressive Approaches
Every coach in this space will encounter clients who want more, more compounds, higher doses, more frequent cycles, more dramatic interventions. This pressure often intensifies when results plateau, when comparison to others (particularly social media content) creates dissatisfaction, or when a client has read about more aggressive protocols somewhere and wants to replicate them.
The communication framework for this conversation has three components. First, validate the motivation: the client wants to make progress, which is why they are working with you. Second, provide honest information about what the marginal gain of escalation actually looks like relative to the risks added, this is where CompoundLab’s compound profiles and interaction analysis are genuinely useful, because they make the risk discussion concrete and evidence-referenced rather than a matter of the coach’s opinion. Third, hold the professional boundary clearly: you will coach responsible, harm-reduction-informed protocols, and protocols that exceed that framework are not something you can support.
The last point must be stated directly, not implied. A client who hears gentle hedging will continue to apply pressure. A client who hears “that is not something I can support in good conscience, and here is exactly why” understands the nature of the limit. Some clients will leave. Those who stay will do so with a clear understanding of what working with you means.
Be especially alert to the escalation dynamic around Trenbolone. It is the compound most commonly at the centre of “I want to add it” conversations before a client is remotely ready. The honest harm-reduction case, that Trenbolone has no approved human medical use, has the most significant cardiovascular and neurological risk profile among commonly discussed compounds, and produces side effects in a meaningful proportion of users that require cessation, is a sufficient and honest foundation for declining to support its use in clients who are not deeply experienced, comprehensively monitored, and fully informed.
The Liability Landscape
The legal framework governing fitness coaching varies by jurisdiction, and this section is educational rather than legal advice. Consult a lawyer familiar with your jurisdiction for specific guidance.
In most common-law jurisdictions, coaches are not licensed healthcare providers and do not hold prescribing authority. The legal risk in the coaching context most commonly arises not from the existence of the coaching relationship itself but from specific actions: recommending specific compounds, doses, or medical interventions; misrepresenting credentials or expertise; failing to refer when referral was clearly warranted; and making claims that imply a therapeutic or medical role.
Practical risk management in this context includes: maintaining clear documentation of your educational rather than prescriptive role; using written coaching agreements that specify the nature of the service (fitness coaching with educational harm-reduction information, not medical advice or supervision); including explicit disclaimers about the nature of any information shared; and building in explicit informed consent processes for clients who are working in a domain with documented health risks.
Insurance is also relevant. Standard personal training liability insurance typically does not cover advice about compound use. Specialist sports coaching or harm-reduction advisory roles may have different coverage options; the specifics depend entirely on your insurer and jurisdiction. The prudent approach is to discuss your practice explicitly with your insurer and ensure you have appropriate coverage rather than assuming standard policy terms apply.
Selected references for major clinical, mechanistic, or protocol claims. Community-practice points may not be cited individually.